Cutaneous warts caused by human papilloma virus (HPV) constitute one of the most common viral infections of the skin and mucosae. After acquisition, the virus remains in the skin indefinitely and may give rise to recurrent lesions, the frequency of which depends upon the HPV serotype and host immunity against the virus. Warts also tend to spread locally around the site of original lesion by autoinoculation induced by trauma-like scratching, called “pseudo-Koebner” phenomenon). Most of the procedures employed for temporary hair removal (THR) such as shaving, threading, waxing, or using depilatory creams result in trivial unnoticeable trauma to the skin. In a patient with pre-existent viral warts, these may seed and spread, whereas in patients not yet exposed to HPV, THR procedures breach the protection of the epidermis and allow viral inoculation from an external infected source, such as a non-sterile razor blade or an infected thread or towel, resulting in fresh eruptions.
Case Description
Case 1: Verrucae Barbae
A 26-year-old man presented with multiple light brown-colored asymptomatic discrete flat papular lesions over the upper and lower neck (Figure 1), which he noticed within two weeks of getting his beard shaved from a local barber to whom he had gone for the first time. He had no history of similar lesions elsewhere in the past. He continued to shave regularly thereafter and noticed a gradual increase in number of lesions in the beard area of the neck. A clinical diagnosis of verruca plana (with spread due to shaving-induced pseudo Koebnerization) was made and lesions were successfully ablated with a bipolar radiofrequency device under topical anesthesia.

Figure 1: Verrucae Barbae: Multiple firm warty papules (verruca vulgaris) over the beard area of a 26-year-old man.
Case 2: Threading Warts
A 35-year-old woman presented with multiple skin-colored 2 to 4 mm sized flat-topped papules localized linearly as a cluster just below the left eyebrow for the last six months (Figure 2). She gave a history of noticing two such lesions below the left eyebrow six months earlier, which had appeared within 15 days of getting threading done at a beauty salon. Although she started doing threading herself instead of going to the salon, the lesions increased in number following each episode of brow-threading. There were no lesions elsewhere. Keeping a differential diagnosis of verruca plana and lichen planus, punch biopsy was performed, which confirmed the diagnosis of verruca plana. Lesions were carefully ablated under topical anesthesia with a bipolar RF device.
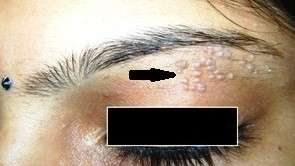
Figure 2: Threading Warts: Multiple skin-colored to violaceous, 2-4mm sized, flat-topped papules arranged linearly near the left eyebrow developed following eyebrow threading.
Case 3: Waxing Warts
A 23-year-old woman presented with a one-month history of multiple, skin-colored, flat, asymptomatic papules over the left shin (Figure 3). She had only three to four such lesions over the upper left thigh region for the past few months. However, numerous new similar-looking lesions suddenly spread over the left shin and lower thigh area within three weeks of waxing the leg. On closer examination of the legs, the lesions were present discretely as well as in a linear distribution suggestive of spread due to pseudo-Koebnerization. There were no similar lesions elsewhere on the body. The patient was unwilling to undergo lesional biopsy. Treatment with tretinoin 0.1% cream recommended for 6 to 8 weeks resulted in good improvement.
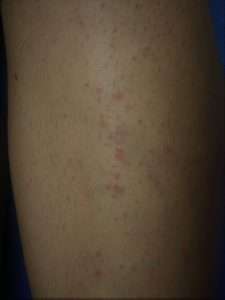
Figure 3: Waxing Warts: Skin-colored to pinkish flat asymptomatic papules clustered unilaterally over the shin of a 23-year-old woman that spread following waxing.
Comments:
First described by Heinrich Koebner in 1877, Koebner’s isomorphic phenomenon is the development of isomorphic pathologic lesions in the traumatized uninvolved skin of patients who have a pre-existing dermatosis. It may occur due to trauma induced by 1) mechanical or thermal trauma and allergic or irritant reactions (e.g., scratching, surgical incisions, needle-punctures, tattooing, shaving, insect-bites, vaccination, tuberculin testing, etc.); 2) dermatoses (e.g., dermatitis, folliculitis, zoster, etc.); or 3) therapy (e.g., radiotherapy, ultraviolet light, laser hair removal, etc.). Boyd and Neldner have classified Koebner’s phenomenon into the following three different groups: 1) true Koebnerization, described in psoriasis, lichen such as warts and molluscum contagiosum; 2) occasional localization (e.g., in Darter’s disease, lichen sclerosus); and 3) questionable Koebnerization in disorders with anecdotal reports (e.g., lichen nitidus, vasculitis, pemphigus vulgaris, etc.). While immunologic factors have been implicated in true Koebnerization, pseudo-Koebnerization represents seeding of surrounding tissues by trauma-like scratching or shaving and recently, threading. Warts are known to spread by seeding into surrounding areas in the beard area of men due to shaving or after tattooing and in women who shave their legs. Shaving has been the standard practice for men for ages to remove their beards and moustaches as well as remove hair from other parts of the body. Despite the use of best quality razors, the process of shaving entails inadvertent breach into the shaved skin allowing for HPV to inoculate from a pre-existing lesion over the face or due to exposure to an infected fomite (e.g., a hand towel). An electrical trimmer is less likely to result in seeding of virus and thus a preferred alternative to razor blade for men with multiple and/or recurrent beard warts.
Threading is the preferred THR used by women themselves at home or more commonly done by beauticians at beauty salons for removal of unwanted hair and eyebrow shaping and enhancing the cosmetic appearance of the upper lip. In this simple procedure, a double-stranded thread is held between both hands and one hand is twisted 5 to 6 times while tightly holding the other section of the thread tightly. Then the thread is converted to a figure 8 with two triangles and one triangle of the thread being placed over the eyebrow from where hair needs to be plucked. Keeping the thread juxtaposed to the hairline, quick opposing scissors-like movements against the direction of hair growth removes the hair. Threading may contribute to the spread of warts in the following two ways: 1) cross-infection from a client who had HPV infection and her thread was re-used for another person, or 2) spread of pre-existing warts if they are located in the threading territory. The snappy scissors-like movements of threading are sufficient enough to breach the protective epidermal barrier and allow HPV inoculation and seeding. To avoid warts due to threading, ideally, ablative removal of the pre-existing warts should be done as soon as possible and threading attempted only after complete healing of lesions occurs. Additionally, a fresh thread should always be used, the area which already contains some lesions should not at all be touched and any fomite suspected to be infected should not be allowed to come in contact with the depilated skin.
Waxing is another popular THR among both the sexes as it provides longer-lasting hair removal. Warm wax is applied to the area and after some time, it is removed (stripping the wax) in the opposite direction of the hair growth, pulling hairs out at the root. Apart from the pain, this THR method also abrades the skin during the stripping of wax.
All of these procedures are causes for inadvertent skin trauma creating a portal for infection. Another unrelated cosmetic practice that is well-known to cause eruption of warts is cosmetic tattooing. An infected tattoo needle is the most likely to inoculate the skin directly through penetration and implant the wart. A few such cases have been reported. Thus, I proposed the broad term “cosmetic warts” for all cases arising out of a cosmetic procedure including THR methods and tattooing.
Treatments commonly employed for these lesions include destructive, chemotherapeutic, virucidal, immunologic, and alternative modalities. Destructive treatments include cryotherapy, radiocautery, topical acids, cantharidin, surgical excision, laser ablation, and electrosurgery. Chemotherapeutic and virucidal therapies include salicylic acid, topical tretinoin, imiquimod, interferons, bleomycin, cidofovir, acyclovir, 5-fluorouracil, formaldehyde, and glutaraldehyde. Immunologic therapies include topical sensitizers, intralesional sensitizers, and cimetidine. Alternative therapies include radiation, acupuncture, ultrasound, hypnosis, localized heat therapy, folk therapies, and homeopathy.
Prevention is always better than cure. Deferring the procedure until pre-existing warts are ablated, or if the procedure cannot be delayed, strictly avoiding that area during the procedure, are of paramount importance. Secondly, beauty salon personnel should be educated about avoiding reuse of threads or blades during threading or shaving, respectively, and to use freshly laundered and hygienic towels on every new client. Tattooing should be carried out in a proper hygienic environment with fresh unused needles.
Moreover, all instruments (e.g., scissors, forceps, and razors) used for threading, shaving, and facials should be properly sterilized to avoid infection. Further, aestheticians should defer such procedures in individuals with vitiligo, psoriasis, lichen planus, bacterial infections, warts, or molluscum.
This article emphasizes the need to educate and sensitize patients, dermatologists and aestheticians about Cosmetic Warts that spread via pseudo-Koebnerization, especially because it is not uncommon and is easily preventable. Further, early ablation of visible warts may substantially reduce the overall burden of further spread of infection.
DISCLAIMER: This article is an informative synopsis of the detailed original article published as: Sonthalia S, Rahul A, Rashmi S. Cosmetic Warts: Pseudo-Koebnerization of Warts after Cosmetic Procedures for Hair Removal. J Clin Aesthet Dermatol. 2015 Jul;8(7):52-6.